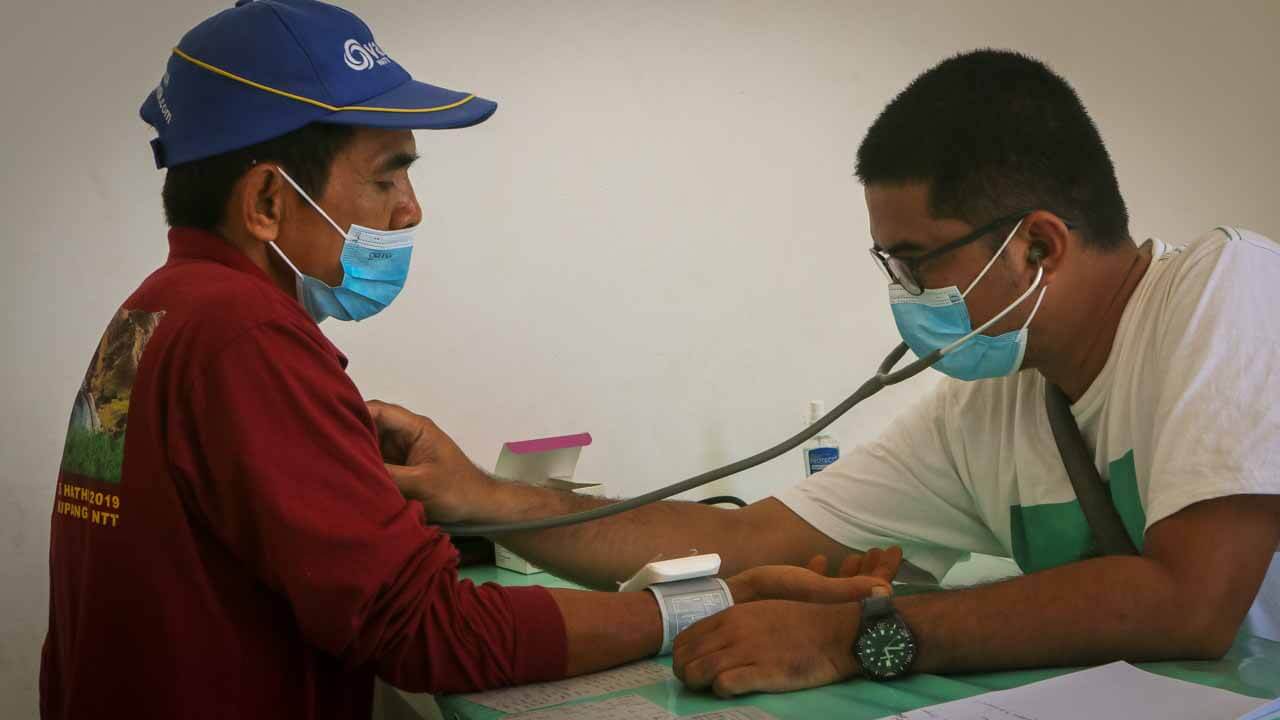
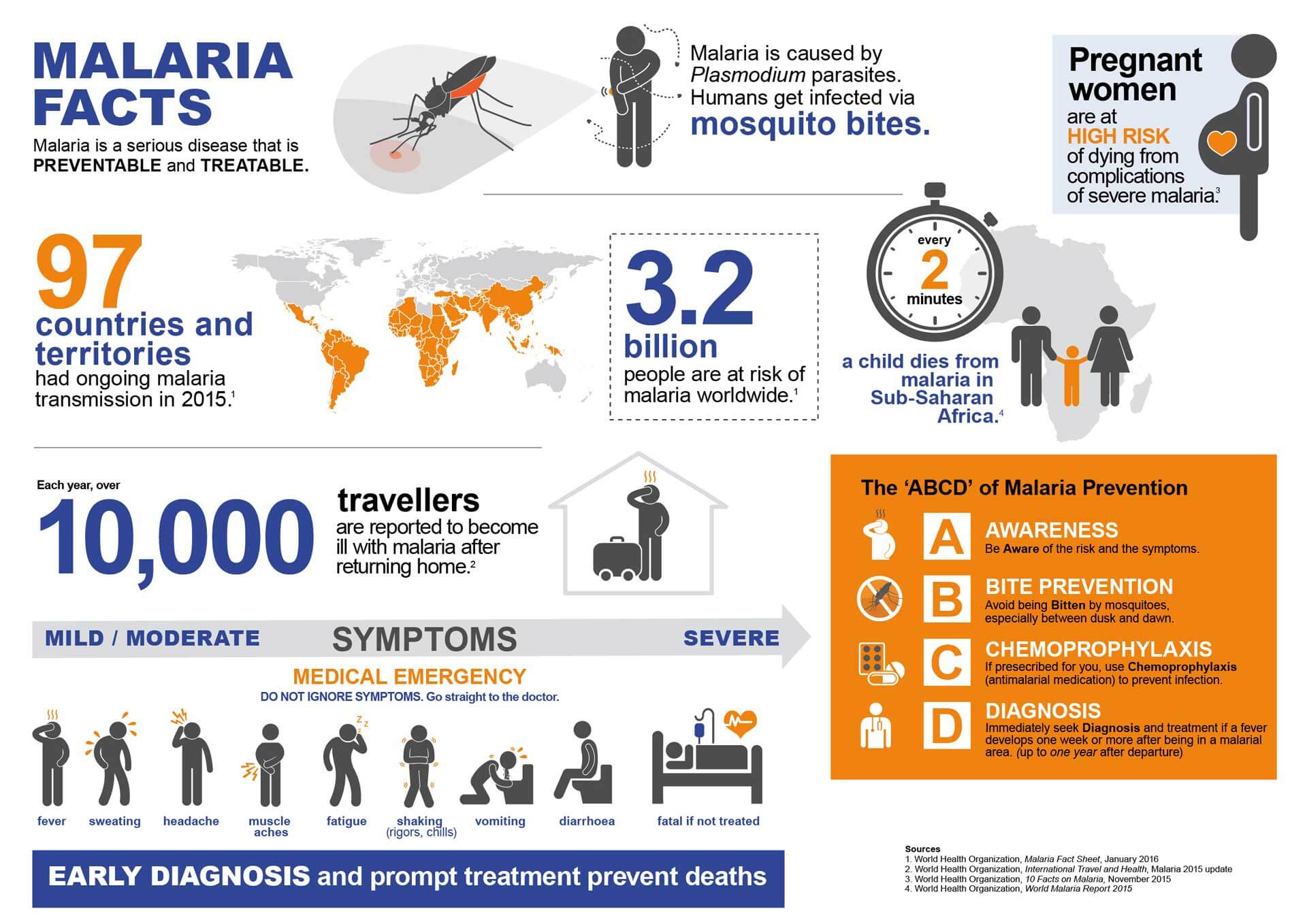
*Malaria is a life-threatening disease that spreads when an infected mosquito, bites a person. The mosquito transfers parasites into that person’s bloodstream. Symptoms of malaria include fever and shaking chills. Malaria is common in tropical countries such as Africa and Asia. Malaria is treatable if it’s caught early.
What is malaria?
Malaria is a serious disease that spreads when an infected mosquito bites a human. Tiny parasites can infect mosquitoes. When it bites, the mosquito injects malaria parasites into the person’s bloodstream.
*What type of mosquito causes Malaria? – The lexicon here
If left untreated, malaria can cause serious health problems such as seizures, brain damage, difficulty breathing, organ failure and death. Malaria is often referred to as the epidemic of the poor while the disease is largely determined primarily by climate and ecology, and not by poverty per se, the impact of malaria wreaks havoc on the poorest, those who can least afford preventive measures and medical treatment.
The impact of malaria is not only felt in terms of human suffering and deaths caused by the disease, but also in terms of the economic impact on areas with high rates.
Malaria is a devastating disease with some 40 percent of the world’s population in 107 countries at risk today. It kills a child every 2 minutes, and some 410’000 people a year – the large majority in the poorest countries!
How common is malaria?
Malaria is common in tropical areas where it’s hot and humid. Worldwide, more than 230 million people get malaria annually, the majority of these cases occur in Africa and South Asia.
What causes malaria?
People get malaria when an infected *mosquito bites them. A *mosquito becomes infected by biting someone who has malaria. The infected mosquito transfers a parasite into a person’s bloodstream, where the parasites multiply. Five types of malaria parasites can infect humans.
In rare cases, pregnant women with malaria can transfer the disease to their children before or during birth. Very rarely, malaria can transfer through blood transfusions, organ donations, and hypodermic needles.
“Malaria and poverty are intimately connected. As both a root cause and a consequence of poverty, malaria is most intractable for the poorest countries and communities in the world that face a vicious cycle of poverty and ill health”. – Fair Future Foundation
Fair Future and Malaria
Although the cases have decreased since 2010, the current situation sees an upsurge in cases of malaria, linked to the economic situation of the country and the crucial lack of access to basic medical care.
In 2020, 256,000 cases of malaria were recorded in Indonesia. This figure should nevertheless be taken in the conditional because in a large number of regions of the country, people do not have an identity card or family record book, or people do not have access to medical care. Mortality, for example in the eastern regions, is still high: Fair Future can regularly notice this during medical visits to the outskirts of the region, or through testimonies from villagers. It should be noted that Alex Wettstein, founder of the Foundation and member of the medical team on site, can attest to this since he himself caught malaria on the island of Flores.
So far, there are still challenges to be overcome as the most worrying challenge is how to reduce the number of cases of active or passive malaria, such as the distribution of mosquito nets and the strengthening of human resource capacities of the medical field areas.
We also note that in some endemic areas people think that malaria is a common disease. And although malaria can be prevented and treated, it can also lead to death. Therefore, the concept of how to prevent this disease from occurring in the community is a challenge for all of us on the ground, today but especially tomorrow.
A challenge simply because medical resources are rare, health centers too far from the villages. People do not own vehicles, the roads are often difficult to navigate. The truck is most of the time the only way to get to a health center, at the cost of a difficult trip, if not impossible for a person suffering from malaria. Read about the “Truck of Life” program here.
Economic cost of malaria on countries
Malaria can be an economic disaster. Countries with high malaria transmission have historically had lower economic growth than countries without malaria. Countries that succeeded in reducing malaria showed substantial growth and improved prosperity thereafter;
- Malaria is estimated to cost millions of dollars in the gross domestic product (GDP) in Indonesia every year. Illness slows economic growth due to loss of life and lower productivity – this is what economists call a “growth penalty”. When it is repeated from year to year, it constitutes a serious constraint on economic development;
- The direct costs of malaria (but also of other diseases such as starvation issues, tuberculosis, Covid-19 pandemic, AIDS, and other childhood diseases such as asthma linked to the air pollution in Indonesia), include high public expenditure to try to maintain the health facilities and infrastructure, manage effective malaria control campaigns and provide public education;
- For countries with a high malaria burden, the disease can account for up to 40 percent of public health expenditure, with malaria accounting for up to 50 percent of outpatient visits;
- The indirect costs of malaria are also widely felt as worker productivity declines with increasing sick leave, absenteeism, and premature labor mortality. For many, the period of malaria transmission coincides with the planting season, further reducing agricultural productivity.
How is malaria treated?
Treatment for malaria should start as soon as possible. To treat malaria, your provider will prescribe drugs to kill the malaria parasite. Some parasites are resistant to malaria drugs. The type of medication and length of treatment depend on which parasite is causing your symptoms.
All malaria infections are serious illnesses and must be treated as a medical emergency. In offering guidance on the choice of antimalarial drugs, the main concern is to provide protection against **Plasmodium falciparum malaria, the most dangerous and often fatal form of the illness.
Atovaquone-proguanil Brand names: Malarone, Malanil and others; generics available.
TAKE 1 TABLET DAILY (ATOVAQUONE 250 mg + PROGUANIL 100 mg).
START 1-2 DAYS BEFORE ENTERING THE MALARIOUS AREA, CONTINUE DAILY DURING YOUR STAY AND CONTINUE FOR 7 DAYS AFTER LEAVING.
Note: Take at the same time every day with food or milk.
Doxycycline Brand names: Vibramycin and others; generics available.
TAKE 1 TABLET DAILY OF 100 mg.
START 1 DAY BEFORE ENTERING THE MALARIOUS AREA, CONTINUE DAILY DURING YOUR STAY AND CONTINUE FOR 4 WEEKS AFTER LEAVING.
Note: When taking this drug, avoid exposure to direct sunlight and use sunscreen with protection against long-range ultraviolet radiation (UVA) to minimize the risk of photosensitive reaction. Take with large amounts of water to prevent esophageal and stomach irritation.
Mefloquine hydrochloride Brand names: Lariam, Mephaquin, Mefliam and others; generics available.
TAKE 1 TABLET OF 250 mg (228 mg base) ONCE A WEEK.
START 1-2 WEEKS BEFORE ENTERING THE MALARIOUS AREA, CONTINUE WEEKLY DURING YOUR STAY AND CONTINUE FOR 4 WEEKS AFTER LEAVING.
Note: Side effects include nausea and headache, including neurological side effects such as dizziness, ringing of the ears, and loss of balance. Psychiatric side effects include anxiety, depression, mistrustfulness, and hallucinations. Neurological side effects can occur any time during use and can last for long periods of time or become permanent even after the drug is stopped. Seek medical advice if any neurological or psychiatric side effects occur.
For further details, cautions, contraindications, or alternatives, including guidelines for pediatric dosages and Emergency Self Treatment, download our whitepaper
How to Protect Yourself Against Malaria.
The recommendations for malaria prophylaxis outlined here are intended as guidelines only and may differ according to where you live, your health status, age, destination, trip itinerary, type of travel, and length of stay. Seek further advice from your physician or travel health clinic for the malaria prophylactic regimen most appropriate to your needs.
If I get malaria, will I have it for the rest of my life?
No, not necessarily. Malaria can be treated. If the right drugs are used, people with malaria can be cured and all malaria parasites can be cleared from their bodies. However, the disease can continue if left untreated or if treated with the wrong medication.
Some drugs are not effective because the parasite is resistant to them. Some people with malaria can be treated with the right medicine.
Two species of parasites, ***Plasmodium vivax and ****P. ovale, have liver stages and can stay in the body for years without causing disease. If left untreated, these liver stages can reactivate and cause malaria attacks (“relapses”) after months or years without symptoms. People diagnosed with P. vivax or P. ovale are often given a second medication to help prevent these relapses. Another type of malaria, P. malariae, if left untreated, is known to stay in some people’s blood for decades.
Pregnancy, preconception and breastfeeding
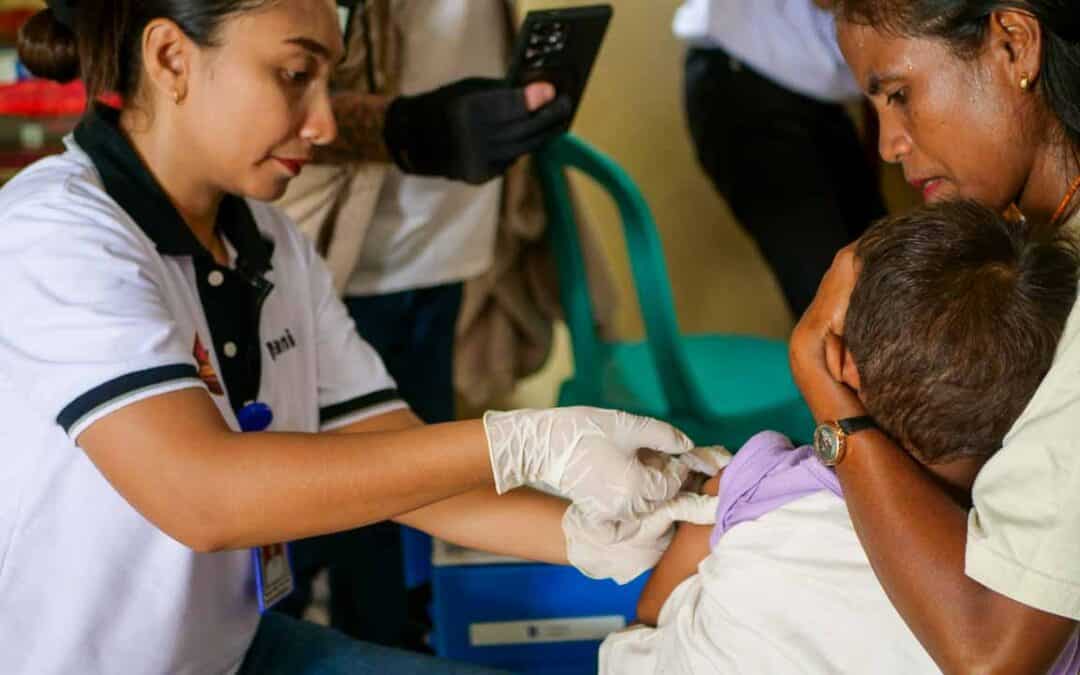
Malaria in pregnant women can be more serious than in non-pregnant women. Malaria can increase the risk of serious pregnancy problems, including prematurity, miscarriages and stillbirths. This phenomenon is exacerbated in the regions where Fair Future works, as people live a precarious life in terms of health, access to water, lack of quality food, lack or absence of medical care and information.
Lexicon
* Usually, people get malaria by being bitten by an infective female Anopheles mosquito. Only Anopheles mosquitoes can transmit malaria and they must have been infected through a previous blood meal taken from an infected person. When a mosquito bites an infected person, a small amount of blood is taken in which contains microscopic malaria parasites. About 1 week later, when the mosquito takes its next blood meal, these parasites mix with the mosquito’s saliva and are injected into the person being bitten.
** Plasmodium malariae is a parasitic protozoan that causes malaria in humans. It is one of several species of Plasmodium parasites that infect other organisms as pathogens, also including Plasmodium falciparum and Plasmodium vivax, responsible for the most malarial infections.
*** Plasmodium vivax is a protozoal parasite and a human pathogen. This parasite is the most frequent and widely distributed cause of recurring malaria.
**** Plasmodium ovale is a species of parasitic protozoa that causes tertian malaria in humans. It is one of several species of Plasmodium parasites that infect humans including Plasmodium falciparum and Plasmodium vivax which are responsible for most malarial infection.
Your comment and feedback is invaluable
…to all of us here who are working in the field. You have a role to play, you can bring us your knowledge, it will be greatly appreciated. Thank you so much for your words and your benevolence.